Poor data collection regarding personal care could be making it easier to commit Medicaid fraud, and the Centers for Medicare & Medicaid Services (CMS) should issue guidance to improve the situation, according to a new report from the Government Accountability Office (GAO).
There are two main systems through which CMS collects data about Medicaid personal care services—the Medicaid Statistical Information System (MSIS) and the Medicaid Budget and Expenditure System (MBES). Both are falling short, the GAO found.
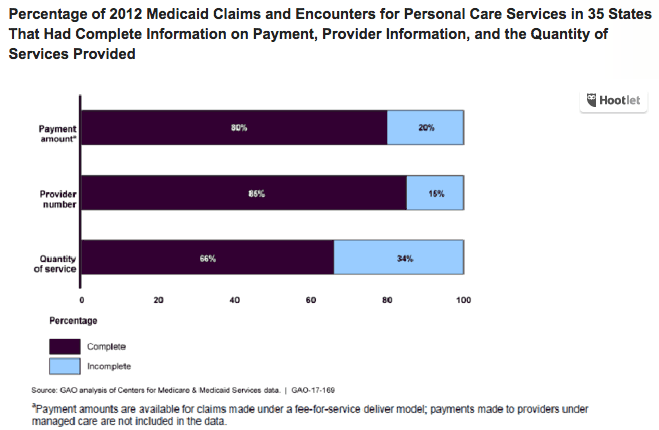
For instance, at the time of the GAO’s investigation, 15% of MSIS claims lacked provider identification numbers, and there were more than 400 different procedure codes used to identify services provided. For the MBES, about 17% of expenditure lines were not reported correctly.
Overall, there were $4.9 billion worth of claims in 2012 that did not identify the person who provided the service, GAO highlighted in a “Fast Facts” release that accompanied the report, which was publicly released Monday.
GAO issued several recommendations in the report, including that CMS should establish standard reporting guidance for personal care, with the goal of states furnishing complete and consistent procedure codes, provider identification numbers, units and dates of service, and other data.
The Department of Health and Human Services (HHS), CMS’ parent agency, already has put out a request for information related to “reforms and policy options” to accelerate home- and community-based services, the agency noted in its response to the GAO. This input may include information on how to better capture some information related to personal care, and HHS will determine what next steps make sense based on the responses to the RFI, the agency stated.
In December 2016, GAO issued a report stating that Medicaid’s patchwork approach to paying for personal care services needs to change.
Written by Tim Mullaney




