Nearly half of home health providers anticipate decreasing their therapy utilization in 2020 in response to the Patient-Driven Groupings Model (PDGM), a payment overhaul from the Centers for Medicare & Medicaid Services (CMS) that is partially designed to refocus the industry toward nursing.
Among its changes, PDGM shifts home health payment away from existing therapy thresholds and toward patient characteristics. Federal watchdogs have suggested in the past that home health providers have grown unfairly profitable because of the over-delivery of therapy services.
“CMS has been saying for several years that we need to do away with this therapy-driven model, even though they’re the ones who came up with it,” J’non Griffin, president of Home Health Solutions LLC, previously told Home Health Care News. “PDGM takes us back to more of a nursing-focused model, not that therapy isn’t important anymore.”
Insight into how home health providers plan to change their therapy strategy in 2020 comes from new survey data compiled by the National Association for Home Care & Hospice (NAHC). The survey features responses from 685 home health providers across the U.S., the majority of which are free-standing agencies.
NAHC President William A. Dombi and Kornetti & Krafft Health Care Solutions owner Cindy Krafft — a physical therapist — highlighted key results during a Tuesday webinar.
“I know, as a therapist, my brothers and sisters in the therapy universe get a little antsy … thinking that [PDGM] is going to be the death knell for therapy and that therapists are all going to lose their jobs,” said Krafft, who co-founded her health care consulting firm along with fellow PT Diana Kornetti.
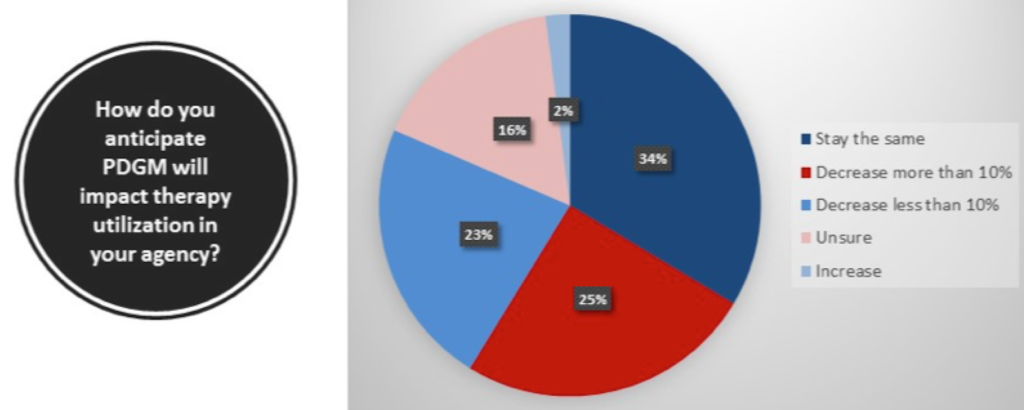
Overall, about one-third of participating home health providers said they plan to keep their therapy utilization the same in 2020, according to the NAHC survey. In contrast, 23% of surveyed providers said they expect to decrease utilization by less than 10% — with 25% planning to reduce it by more than 10%.
About 16% of participating home health providers said they were unsure as to how PDGM will affect their therapy operations. Only 2% said they plan on increasing therapy utilization in response to the payment overhaul.
The fact that some respondents reported being unsure about PDGM’s therapy impact shouldn’t be interpreted as a sign of those providers being unprepared, Dombi said. Rather, it signals the industry avoiding any “knee-jerk reactions.”
“That does not mean they’re unprepared,” he said. “It may mean that their preparation is taking a little bit more time, or they’re waiting because adjustments are ongoing.”
Washington, D.C.-based NAHC is a nonprofit advocacy organization that represents more than 33,000 home care and hospice organizations.
In addition to gauging the broad change in utilization post-PDGM, the NAHC survey also gathered information on home health provider’s views on adopting remote patient monitoring and other telehealth tools specific to therapy.
Once PDGM goes live, providers will generally need to become more cost-sensitive when delivering therapy services in the home setting. Used appropriately, experts say, telehealth tools can eliminate the need for certain in-person therapy visits without negatively impacting patient care.
More than one-quarter of home health providers that participated in the NAHC survey said they are actively exploring telehealth technology specific to therapy. More than 5% said they anticipated an increased use of therapy telehealth tools in 2020.
“I think that a lot of the telehealth conversation that we know it today — with remote monitoring — has always been packaged in-line with, ‘This will reduce your nursing visits,'” Krafft said. “There’s been technology similar to that for rehab for a long time, yet it hasn’t really found it’s way into home health, I believe, because the perception was using this technology might decrease my therapy visits. In the PPS [model] that stands today, decreasing therapy visits wasn’t necessarily seen as financially a good idea.”
PDGM may open the floodgates, she said.
Companies featured in this article:
Home Health Solutions LLC, Kornetti and Krafft Health Care Solutions, National Association for Home Care & Hospice



