Older adults living with dementia at home tend to be sicker and more socially complex than their counterparts in senior housing communities and nursing homes, a new study has found.
That means home care providers that have branded themselves as specialized dementia experts likely have their work cut out for them.
In the United States, more than 5.7 million adults older than 65 live with Alzheimer’s disease and related dementias. Of those, roughly one in three seniors eventually dies with some form of dementia, according to the Alzheimer’s Association.
Despite the rising prevalence and the preference of older adults to age in place, relatively little is known about the health and social characteristics of the at-home dementia population, University of California San Francisco researcher Krista Harrison told Home Health Care News.
“Much of the research on care for people with advancing dementia focuses on end-stage or advanced dementia in nursing homes,” Harrison said. “However, both my personal and professional experience [suggest] that many people live at home with dementia even when things get hard — and intense caregiving needs can last for years.”
To learn more, Harrison and a team of researchers analyzed the medical characteristics of 728 adults over the age of 65 with moderately-severe dementia across three settings: individuals’ homes, residential care and nursing homes. Residential care spanned the spectrum of retirement communities, from those offering health care support at extra cost to assisted-living facilities.
Results were published in a Journal of the American Geriatrics Society study on Wednesday.
Of the 728 adults included in the study, 499 lived at home, with 126 living in residential facilities and 103 in nursing homes. Broadly, researchers found, older adults living at home with moderately-severe dementia had an overall worse picture of health, displaying higher rates of co-morbidities and dealing with more regularly bothersome pain.
For example, 32.3% of at-home individuals had five to 10 co-morbidities. That’s compared to 15.3% and 29.5% of those in residential care settings and nursing homes, respectively.
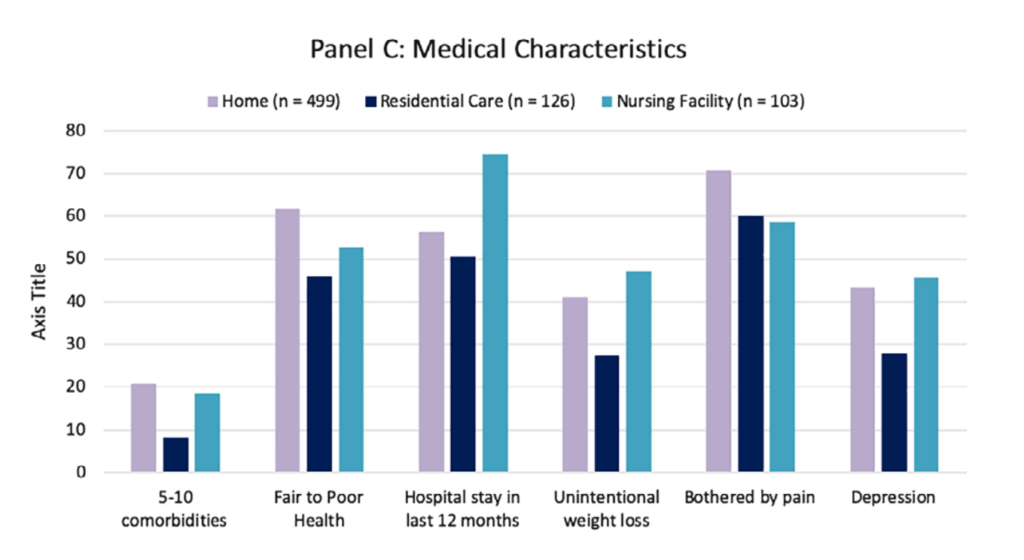
Additionally, older adults living at home with moderately-severe dementia were more likely to be black, not born in the United States and to have less educational attainment than those in residential care or nursing homes.
“People living at home also have high rates of hospital stays in the prior year, depression, unintentional weight loss, and falls or fall concerns,” Harrison, who served as lead author of the study, said.
Seniors living in residential care had higher incomes and were more likely to be U.S.-born and have post-high-school education, compared to those living at home or in nursing facilities. Conversely, the group was less likely to be married or living with someone compared to those living at home or in nursing facilities.
In 2018, the median monthly cost of assisted living in the United States was $4,000 — or $48,000 annually.
Over the past few years, an increasing number of at-home care providers have launched specialized service lines to care for older adults with dementia. Just a few of them, for example, include nationwide franchise giants Right at Home and Interim HealthCare, in addition to Cypress HomeCare in Arizona.
Harrison hopes her research will help steer these and other providers in the right direction to ensure high-quality care.
“[My hope is] this study will help agencies care for people with dementia in their homes and better understand the characteristics of the population more generally, which will help them attend to social, functional and medical aspects of well-being of their clients,” she said. “Staff in home health and personal care agencies may benefit from training in geriatrics and palliative care approaches, which focus on preventing, mitigating, adapting to functional impairment, sources of distress, and ensuring care plans are based on the values and goals of the person with dementia and their family or friends.”
Additionally, Harrison said, tailored training may also help staff understand the experiences and needs of clients who may have low health literacy, be living in poverty or facing other forms of structural disadvantage.
“Ideally, all people with dementia and caregivers would be able to obtain interdisciplinary care in their homes — personal care, social support, help with functional impairments and medical needs,” Harrison said. “[Home care] agencies partnering with home-based medical care programs — both primary care and palliative care — will help achieve this goal.”
Companies featured in this article:
Journal of the American Geriatrics Society, University of California-San Francisco



