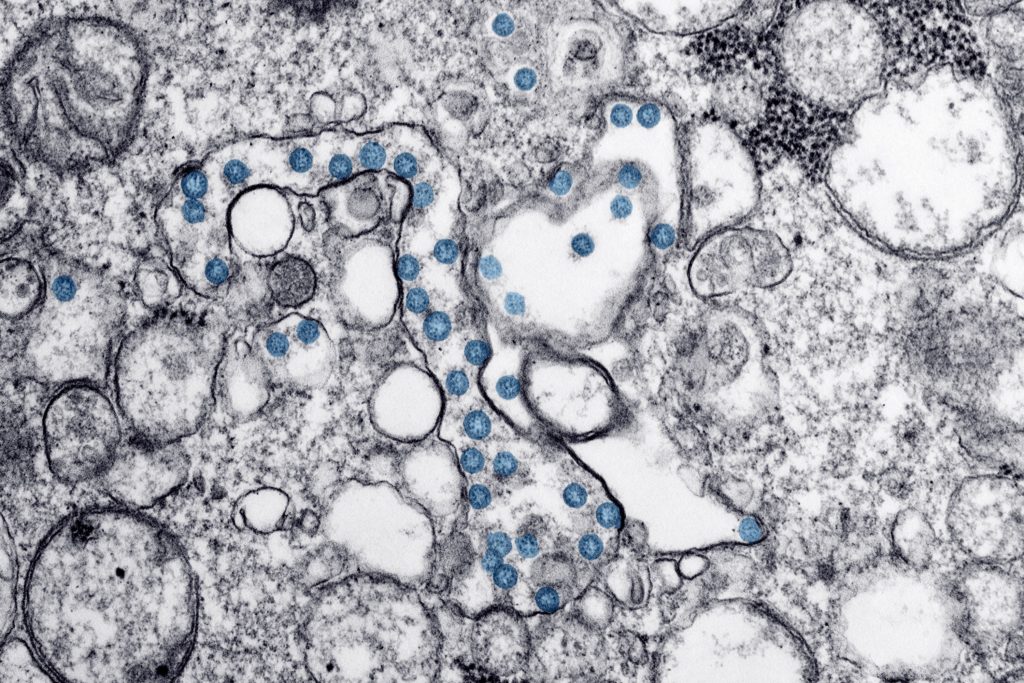
COVID-19 — the viral disease more commonly known as the coronavirus — is spreading. Already, concern has grown throughout the senior living and skilled nursing spaces, especially after confirmed cases surfaced at a Kirkland, Washington-based long-term care facility.
The home health care industry has also started to prepare for possible disruption.
“People have been asking me, ‘Where are we with the coronavirus?’” National Association for Home Care & Hospice (NAHC) President William A. Dombi said Tuesday, speaking at the Illinois HomeCare & Hospice Council’s annual conference. “It’s scary.”
As of Wednesday morning, there were at least 80 confirmed COVID-19 cases in the United States, according to the U.S. Centers for Disease Control and Prevention (CDC), though some reports have that number above 130. Deaths linked to COVID-19 have reached nine, with at least seven having ties to the Washington long-term care facility.
Globally, the coronavirus has infected more than 94,800 people in at least 77 countries, making it one of the most devastating public health crises in recent memory. The worldwide death toll has surpassed 3,000.
It’s still too early to conclusively say how home health providers will be affected by the spread of COVID-19, but industry insiders are beginning to think through the most likely scenarios.
Perhaps most immediately, home health providers may face a shortage of supplies. To avoid that, providers should start checking with their vendors about the continued flow of masks, medication and other key items.
Besides reinforcing their supply line, providers should also review their current emergency response plans and personnel policies, updating both for possible coronavirus outbreaks in their markets.
From a workforce perspective, immediate preparation steps additionally include planning for worker shortages, cross-training staff members and developing family contingency plans.
NAHC released a comprehensive coronavirus checklist on Wednesday. The list — produced with expert advice from Barbara Citarella of RBC Limited Healthcare & Management Consultants — includes several other actions providers should be taking right now.
“As typical with home health and hospice, there’s no panic in the streets about this,” Dombi said. “It’s all about how do we do things right.”
[Take HHCN’s Survey: Analyzing Home-Based Care Industry Impact of Coronavirus]
Keeping calm in moments of crisis is a strength for many home health providers, some of which routinely deal with natural calamities like flooding, tornadoes and hurricanes while caring for patients.
Doing the same with coronavirus will be essential, long-time industry executive Raj Kaushal told Home Health Care News.
“The first thing home health providers must do is educate their staff,” said Kaushal, formerly chief clinical officer at Almost Family. “Building awareness is extremely important generally, but it’s also important so there isn’t panic among health care workers. Companies must designate time to educate their workers on symptoms, prevalence and how to identify patients and properly screen them.”
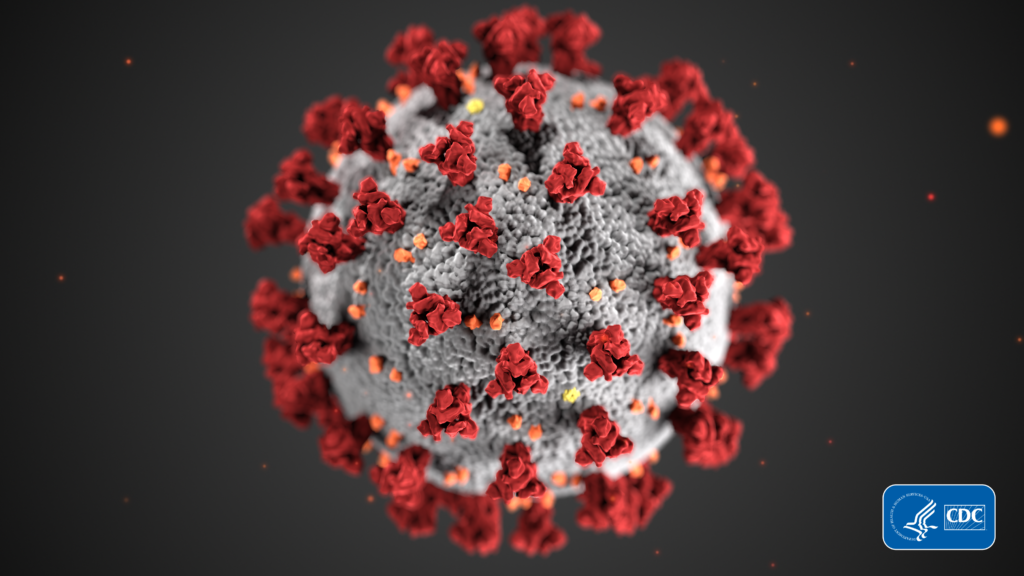 CDC
CDC‘This is real stuff’
Within the United States, at least 13 states have reported coronavirus cases, with the bulk of reports coming out of Washington and California. Reported illnesses have ranged from mild symptoms to severe illness and death, with common symptoms including fever, cough and shortness of breath.
Life Care Center of Kirkland became the first senior care provider to face COVID-19 cases last week. In addition to the at least seven deaths tied to the facility as of Tuesday evening, dozens of other residents and staff members are reportedly experiencing symptoms.
Senior living and skilled nursing operators are among the only groups to regularly provide updates on how the flu impacts their businesses. As a result, operators are well-versed in disease and infection control.
But even they are preparing for worst-case scenarios, as the death rate for COVID-19 appears to be higher than that of the flu.
“I think the effects could be devastating,” Dr. Kevin O’Neil, the chief medical officer for Affinity Living Group (NYSE: ALG), told HHCN sister site Senior Housing News. “And that’s why I think it’s so important that we be really aggressive right now about these infection control measures.”
The Centers for Medicare & Medicaid Services (CMS) announced several actions it’s taking to limit the spread of COVID-19 on Wednesday. Among the actions, CMS is directing state survey agencies and accrediting organizations to focus inspections exclusively on issues related to infection control as well as other serious health and safety threats.
“Today’s actions, taken together, represent a call to action across the health care system,” CMS Administrator Seema Verma said in a statement. “All health care providers must immediately review their procedures to ensure compliance with CMS’s infection control requirements, as well as the guidelines from [CDC].”
Dombi noted that at least one NAHC member has already been affected by COVID-19: EvergreenHealth, which is also based in Washington.
“This is real stuff,” he said.
Depending on how COVID-19 develops in the U.S., home health providers may want to begin preparing for a sudden influx of patients. As the virus spreads, many hospitalized individuals will likely have a need for home health services after discharge.
“[Home health providers] will face that unfortunate opportunity, but what the limiting factor usually is in those situations is capacity,” said Kaushal, who most recently served as president of LHC Group’s southeast division until leaving at the end of last year. “Capacity because of the limitation of supplies and also manpower.”
Furthermore, those who are simply homebound and under observation may also need home-based care services.
“As more areas see community spread, local communities may start employing tools that encourage social distancing,” Dr. Nancy Messonnier, the director of CDC’s National Center for Immunization and Respiratory Diseases, said in a Tuesday news conference. “The goal of social distancing is to limit exposure by reducing face-to-face contact and preventing spread among people in community settings.”
Industry burden
Home health providers previously proved their mettle during the SARS outbreak in 2003 and again during the H1N1 pandemic in 2009.
Both outbreaks were “very disruptive” at times, Kaushal said, noting that a major challenge was sorting through the facts and fictions that circulated throughout the home health workforce.
“But one of the biggest differences between [H1N1 and SARS] is this outbreak is seeing a mortality rate that is potentially higher,” he said. “So the burden on us as an industry to protect our patients and equally protect our employees is much higher.”
Since leaving LHC Group, Kaushal has since launched a care management company, Senior Healthways Inc.
The coronavirus may impact far more than clinicians and patients, too. Rising anxieties over its spread led to the largest single-week stock market downturn since 2008 last week, wiping out $6 trillion in market value.
Companies featured in this article:
CDC, CMS, Illinois HomeCare & Hospice Council, NAHC, National Association for Home Care & Hospice, Senior Healthways