More patients that can be categorized as clinically complex are being referred to home-based care providers. As a response, providers are making moves to ensure that they’re in a position to deliver appropriate care to these patients.
Broadly, this trend has been visible to most home health providers for years. It was exacerbated, however, by the pandemic and a reduction in the availability of acute care.
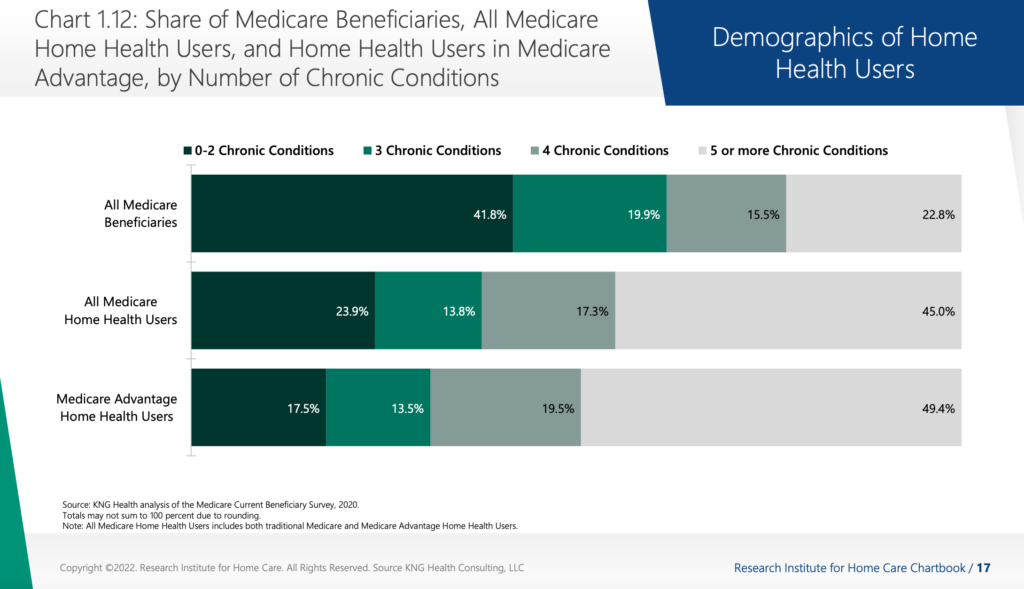
Thus, home health providers have been caring for patients that traditionally still would have been in acute care facilities.
“Over the last three years, starting with COVID and transferring out of that, we’ve seen patients come to us that are certainly more clinically complex,” Blake Nelson, director of home health care at Hamilton Health Care System, told Home Health Care News. “We saw a need to come alongside the hospital when it came to throughput. When COVID patients were coming to the ED and then being admitted and staying at the hospital for 5,6,7 weeks, we saw a need for us to stand in the gap.”
Serving northwest Georgia, Hamilton Health Care System includes a community hospital, medical center and a physician group. The organization also offers long-term care and hospice, as well as home health services through Hamilton Home Health.
At the time, Hamilton Home Health created a COVID Max program focused on relieving pressure off the ED. The program would eventually branch out to tackle diagnosis-related groups that the hospital tends to struggle with, such as chronic obstructive pulmonary disease (COPD) and congestive heart failure (CHF) patients.
Over the last year, Hamilton Home Health has created different “Max” programs focused on COPD, CHF and diabetes.
“The diabetic patients have other comorbidities,” Amanda Horne, clinical manager and administrator at Hamilton Home Health, told HHCN. “They often have non-healing wounds that we’re dealing with. Some of the sickest COVID patients who are in the hospital for extended times are coming out with pressure ulcers. We see a wide array of issues. I would say that people with COPD, CHF and diabetes are the ones that typically have the most issues.”
In addition to new programs, Hamilton Home Health has made other adjustments to meet the care needs of clinically complex patients.
“We’ve had to get creative,” Horne said. “Specifically with CHF, we had to think about what we could do to help those patients stay at home. We would give them more nursing visits, and we were purchasing digital scales for our patients. We would call their cardiologist for them, set up appointments and make sure their transportation is in order.”
Ultimately, strong communication has been a key factor in helping Hamilton Home Health manage its patient volume.
“Communication across the entire system was important,” Nelson said. “From the handoff, to making sure we have a good picture of what’s going on with this patient, so that our clinicians are ready to meet the patient out in the home.”
Hamilton Home Health’s various Max program teams have also been meeting monthly.
“Different thought leaders from inside the system get together and talk through how that program is progressing, and what questions, concerns or issues we may be thinking about, to stay ahead of what may come down the road,” Nelson said.
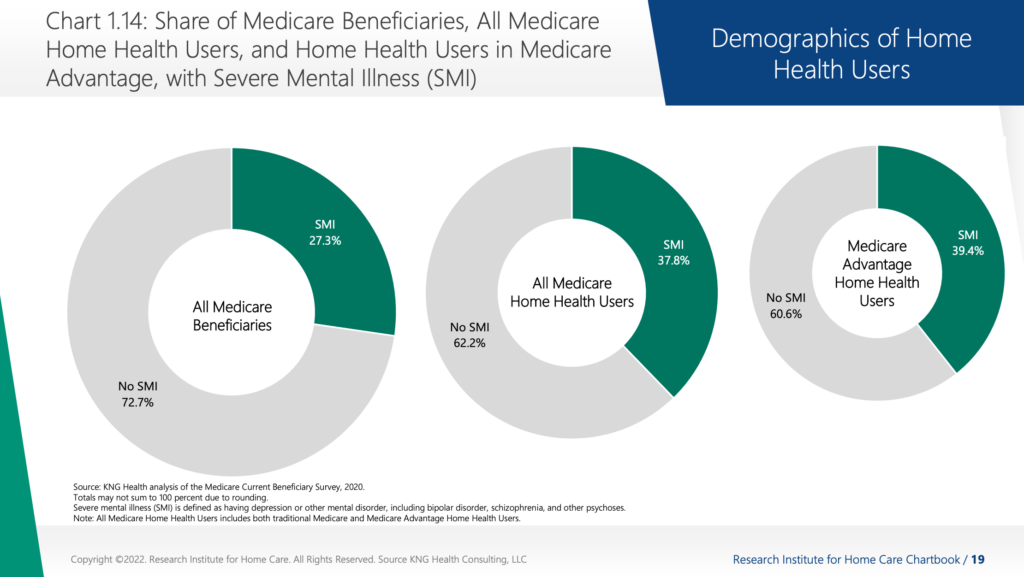
Interim leverages its full care continuum model
At Interim HealthCare, ensuring that the organization is providing a full continuum of care in each of its markets is top priority.
As such, the organization was uniquely positioned to meet the needs of increasingly clinically complex patients.
Based in Sunrise, Florida — and a part of Caring Brands International — Interim is a franchise that provides home health, hospice and palliative care services. The organization is just shy of 600 locations in the U.S. and internationally.
Similar to Hamilton Home Health, Interim is seeing an influx of more patients who are at the higher end of its full continuum of care. This is because length of stays at hospitals are shorter, according to Jennifer Sheets, CEO and president of Interim.
“People are coming home much more acute than they have in the past,” she told HHCN. “We’re seeing, for example, people sent home much quicker after cardiac procedures, after acute heart attacks and strokes.”
Interim is seeing the most clinical complexity come from individuals dealing with multiple comorbid conditions across one or more body systems.
“If you take something like [CHF] and it’s layered on top of cognitive impairment, like dementia, it becomes much more complex,” Sheets said.
A few years back, Interim developed what it calls its Home Life Enrichment standard of care. It’s an approach that continually assesses the evolving needs of Interim’s patients.
Since seeing this increase of higher acuity patients in the home, Interim has doubled down on that philosophy of care.
As a result, the company has invested heavily in certifications and additional education for its clinicians.
“The ability to have clinicians top up their skills, if they’re seeing, for example, more neurologically focused diagnoses coming home, they can top up on that specific education,” Sheets said. “Clinicians also have more real-time access, through devices, to best practice policy and procedures for cases they may not see all the time.”
This wave of more clinically complex patients is also top of mind when Interim looks to recruit new clinicians.
“We do balloon pumps, as people are waiting for open heart surgery, we do chemotherapy infusions, very high acuity things that people who have worked in the ICUs, for example, are used to seeing,” Sheets said.
Even though Interim has made moves to accommodate these patients, Sheets also pointed out that caring for clinical complex patients is part of the company’s history.
“Interim was the very first company to bring home a high-acuity, ventilator dependent child, and that goes all the way back to 1970,” she said. “We were also the first company to bring home a high-acuity ventilated adult, the following year.”




