States with home- and community-based services (HCBS) providers are facing an uphill battle when it comes to implementing service offerings and evaluating the success of their programs linked to the federal funds from the American Rescue Plan Act (ARPA).
That’s according to a new brief that explores how states are assessing the outcomes of their HCBS projects, many of which were and are bolstered by significant federal investments under the ARPA.
The authors of the brief — Alissa Halperin with Halperin Health Policy Solutions and Anne Jacobs with Riverstone Health Advisors — detailed how many providers are struggling with the compressed timeframe of the federal approval process.
Halperin Health Policy Solutions and Riverstone Health Advisors are two health care policy and consulting firms.
In putting the brief together, state leaders told the authors that the spending period around funds poses significant challenges in implementing and evaluating ARPA HCBS initiatives.
“Without fail, every focus group state called out the many challenges introduced by the timing of the federal approval process and spending period,” the authors wrote. “The compressed timeframe within which to create, plan, implement, complete and evaluate their initiatives does not afford enough time, experience and data for fully evaluating the efficacy of many initiatives.”
To understand states’ approaches to evaluating their ARPA spending plan initiatives, the research team conducted a survey with 14 individuals from nine states who played “key roles” in ARPA HCBS implementation.
The brief offers a real-time assessment of states’ successes and challenges in spending ARPA funds while focusing on their evaluation efforts.
The evaluation comes on the heels of the U.S Centers for Medicare & Medicaid Services (CMS) releasing ARPA state spending plans, indicating $36.8 billion was allocated across all 50 states — with $24.6 billion specifically earmarked for direct care worker recruitment and retention activities.
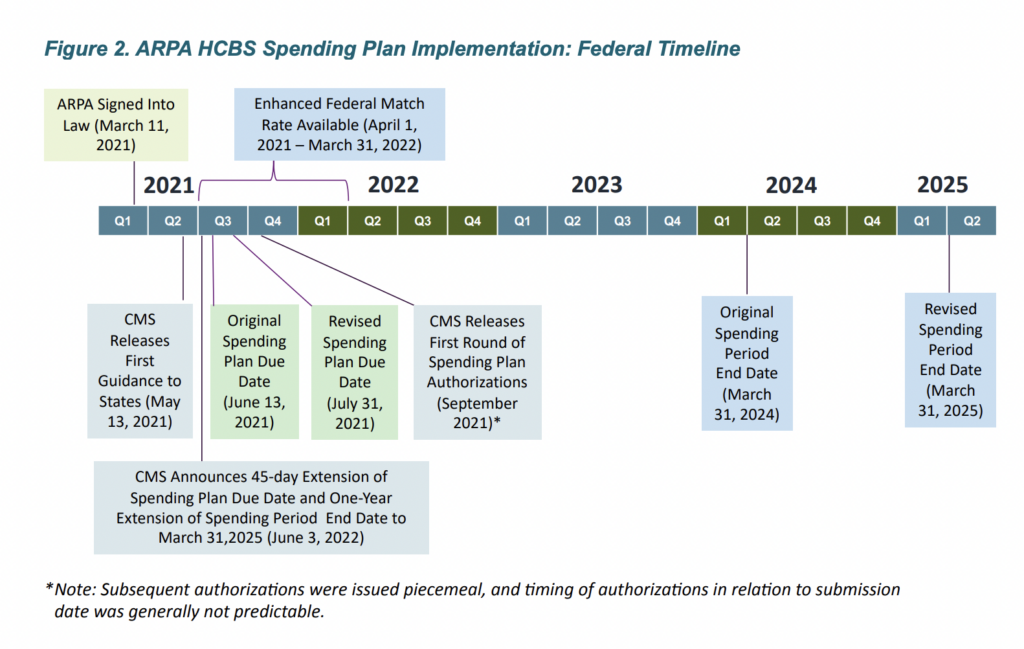
In the spring of 2021, states were given about 10 weeks — extended from the original
30-day timeframe — to develop proposed ARPA HCBS spending plans to submit to CMS.
“We observed first-hand as many states furiously grabbed at any innovative new ideas they could identify, many of which were previously under- or untested,” the authors wrote. “However, the compressed timelines presented a significant challenge to most states’ administrative and program design capacities. They had limited time and resources to be thorough and contemplative in developing their spending plans and to efficiently expand HCBS services, populations, and infrastructures.”
Halperin and Jacobs argue that the rush to propose initiatives under the ARPA HCBS funding did not prioritize evaluation. Instead, the requirements for spending plans were focused on creating new initiatives, maintaining effort levels and reporting progress and spending.
There was no mandate for fully formed plans or evaluations to assess the impact of these initiatives. The tight timeline for proposing, designing and implementing initiatives made it challenging for states to conduct meaningful evaluations.
Several states also faced challenges from their respective state legislatures, which were reluctant to approve initiatives with time-limited funding, like provider rate hikes or eligibility expansions.
Recommendations
For those states and providers that have yet to implement these initiatives under the ARPA HCBS umbrella, the brief’s authors did have a few suggestions.
Making sure there is room for evaluation is Rule No. 1, the authors wrote.
Prioritizing evaluation resources, being transparent in the evaluation process, sharing results regularly to inform future policymaking, setting expectations for the possibility of some projects not achieving desired results and engaging expert evaluators in the process were among the other recommendations.
Companies featured in this article:
Halperin Health Policy Solutions, Riverstone Health Advisors